How the Liver Works
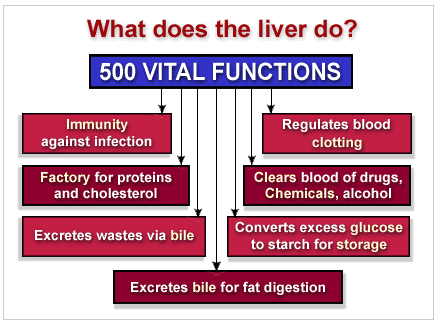
How the Liver Works
The liver, the second largest organ (only the skin is larger), is like a sharp-eyed bouncer guarding the red velvet rope in front of an exclusive nightclub called Your Body: It makes sure the right elements get in and the wrong eliminated.
The liver enforces its stringent standards for good health using an intricate of highly sophisticated cells designed to synthesize, transform or detoxify nutrients and other chemicals in the blood.
Linked to the digestive tract through a complex system of blood vessels, the liver takes nutrition from food in the intestines and changes it into essential nutrients such as proteins, fats and vitamins.
The liver also stores vitamins and sugars (carbohydrates) so the body can have a ready supply in times of need; and it contains and converts iron and iron-related molecules into heme, the main oxygen-transporting molecule in red blood cells. No wonder the immune system, digestive tract, kidney, brain, cardiovascular system and the regulation of sex hormones are all dependent on a healthy liver.
Understanding how the healthy liver works is essential to understanding what happens to the body when hepatitis C prevents the liver from
doing its job.
Blood Circulation and Filtration
The liver has the most complicated network of arteries, veins and capillaries of any organ. In fact, a gallon of blood passes through it every 2.6 minutes.
There are two main vessels that transport the blood:
The portal vein carries all the blood in the large and small intestines to the liverand that brings 90 percent of all the nutrition extracted from food in the intestines through the liver’s processing plant.
The hepatic artery, a branch of a main heart artery called the aorta, brings oxygenated blood from the heart to the liver. Sometimes up to a quarter of all the blood in the body is circulating through the liver.
The portal vein and the hepatic artery are fed by a system of smaller blood conduits that run throughout the liver. These smaller blood conduits in the liver are called sinusoids.
The liver cells, called hepatocytes, are assembled into cordlike structures that are separated by the sinusoids. These hepatocytes and the sinusoids are contained inside lobules, tiny six-sided structures about one-fifth of an inch wide. Each lobule is dense with blood vessels; a vein runs through its center and is connected to the sinusoids, and six or seven additional blood vessels cluster around each lobule. These vessels include branches of the portal vein (that connects the liver to the digestive tract) and the hepatic artery (that connects it to the heart).
The role of all these blood vessels is to bathe the liver cells with toxins, nutrients and other chemicals; the liver cells respond appropriately, excreting bile, synthesizing, breaking down, storing or transporting each element as needed to keep the body healthy and the blood circulating.
In liver disease, scarring of the liver tissue can interfere with the circulation of the blood; this in turn can produce high blood pressure in the portal vein and interfere with the cleansing and nutrition-building functions of the liver.
Bile Production and Fat Metabolism
One to two quarts of bilethe most important digestive chemical in the bodyare synthesized in the liver every day. After you eat a meal, bile made in the liver travels to the major bile ducts and is temporarily stored in the gallbladder until it is needed. When summoned to help with digestion, it travels on through the pancreas and into the intestines, where it breaks down fat molecules so the body can digest them more effectively or excrete them if they are in oversupply. This process allows the body to absorb the oil-soluble vitamins A, D, K and E.
Bile helps the body balance cholesterol90 percent of which is synthesized in the liver, not derived through the food you eat. Blood levels of this fatty substance, essential for healthy cell membranes and production of sex hormones, can surge in hepatitis C. This happens when bile production is impeded by cirrhosis or when scarring of the liver reduces the number of active cells available to process cholesterol or makes it difficult for the cells and the blood in the sinusoids to come into contact.
Bile also helps transport the toxins that the liver neutralizes to the kidneys and intestines for excretion.
When bile flow is impaired because of a blocked bile duct (a possible result of gallstones or scar tissue), the whole body is thrown out of kilter: Vitamin synthesis may be reduced, and toxins cleared though the bile may not be excreted from the body. As a result, a person becomes lethargic or depressed, or experiences fuzzy thinking. Jaundice may set in.
The connection between the liver, bile and feeling down in the dumps has been known for thousands of years. Ancient Greeks coined the word melancholyit literally means black bileto describe a state of overall sadness and world weariness. Chinese medicine doctors have long diagnosed Liver Qj Stagnation when a person has similar symptoms: depression and apathy.
Blood Sugar Regulation
The liver changes glucose (sugar) into glycogen, which it stores until the body needs to regulate blood sugar levels and provide energy to the muscles and the brain. In addition, it helps balance amino acids, the building blocks of proteins that are converted into fatty acids and glucose. In Chinese medicine this is associated with the functions of the Spleen Organ System, which encompasses all pancreatic functions.
Changes in blood glucose levels can indicate liver function problems. In fulminant liver failure (that is, sudden liver shutdown) blood sugar levels drop; with cirrhosis, blood sugar levels may skyrocket as a result of increasing insulin resistance and the development of diabetes.
Toxin Removal
Many toxins such as DDT are lipid soluble; that is, they dissolve in fatty substances, not in water. The liver, using enzymes produced in the liver cells, transforms these fatty toxins circulating in the blood into water-soluble toxins so that they can enter the gastrointestinal and kidney systems and be excreted through the bladder and intestines.
The liver also breaks down natural waste by-products of cell metabolism and other naturally occurring bodily toxins such as ammoniathe by-product of muscle and amino acid metabolisminto less toxic substances (in this case, urea) that can pass through the kidney and become waste.
Bilirubin, a waste product that comes from a breakdown of heme, the central oxygen-carrying molecule in red blood cells, can also act as a toxin. If not cleared out by the liver, this yellowish liquid can produce jaundice, the most vivid symptom of hepatitis and often the first one that alerts a person to the presence of the disease, especially in acute hepatitis or late-stage chronic hepatitis.
The liver also detoxifies drugs, such as clearing aspirin from the blood, breaking down alcohol so it can pass from the system and keeping acetaminophen from being converted to toxic molecules. Excess alcohol harms the liver because it overwhelms the detoxification process, allowing poisons to remain in the liver and damage the tissue.
The liver regulates hormones; hepatitis C disrupts the liver’s ability to keep estrogen levels in check. As levels rise in both women and men, complications occur. In men they may include testicular atrophy and breast development.
Liver Enzyme Synthesis
The liver is awash in enzymes, molecular agitators that are essential for the organ’s important work of transforming chemicals and synthesizing nutrients. AST (aspartate aminotransferase) and ALT (alanine aminotransferase) are liver enzymes used for amino acid metabolism, a process that balances the types of amino acids available for building proteins and then transforms them into proteins. (Tests for AST and ALT enzyme levels are frequently used in diagnosing hepatitis C, despite the fact that they are only crudely indicative of what is going on in the liver: The best use of these tests is to keep tabs on changes in liver inflammation. When ALT or AST levels increase by a factor of ten or more, it can indicate a worsening of the disease.) Note: AST used to be called SGOT, and ALT used to be called SGPT; some labs still use that terminology.
Other enzymes made in the liver that are vital to maintaining overall health include alkaline phosphatase and GGT (gamma-glutamyltransferase). Alkaline phosphatase is involved in phosphorus metabolism, which also delivers energy to the body’s cells. GGT is used in metabolizing another amino acid, glutamate, which affects tissue oxidation. When fatty deposits cause damage to bile ducts or blockages, these enzyme levels increase. Although the elevated levels aren’t necessarily associated with symptoms, blood tests that track these levels can be used to determine the presence and degree of liver inflammation.