What Is Hereditary Hemorrhagic Telanglectasia (HHT)
What Is Hereditary Hemorrhagic Telanglectasia (HHT)
Hereditary Hemorrhagic Telangiectasia (HHT) is a genetic disorder that affects about one in 5,000 people and causes arterial blood to flow directly into the veins, creating weakened ballooned vessels that can rupture. Interventional radiologists are one of the few specialists who can permanently treat this disease that affects approximately half a million people worldwide. As vascular experts, interventional radiologists perform embolization – blocking the blood flow to the affected area – to prevent a life-threatening rupture.
Most patients with HHT function normally and 40 percent have brain or lung involvement that may lead to unexpected severe complications. Physicians treating complications often don’t realize that the underlying disorder is HHT. As a result, most patients are undiagnosed.
Overview of Circulatory System and HHT
In the normal circulatory system, arteries take oxygenated blood from the heart and push it out to all parts of the body under high pressure, while the veins return the blood back to the heart. Small capillaries typically connect the arteries to the veins. A person with HHT lacks capillaries in a few blood vessels in critical locations. Arteries connect directly into veins, creating a fragile site that can rupture and bleed. These abnormal blood vessels are called telangiectasis (tel-AN-jee-eck-TAZE-ee-ya) if they involve small blood vessels (nose, stomach and small bowel) and arterioveneous malformations (AVM) if it involves a larger blood vessel (lung, brain and liver). Telangiectases often occur near the surface of the skin like the mucous membrane in the nose while AVMs appear in the internal organs of the body.
HHT Symptoms Vary With Location
The location of the telangiectases or AVM impacts what problems a person with HHT might face. A person with abnormal GI tract blood vessels should watch for black stools and anemia that can cause fatigue, shortness of breath, chest pain or light-headedness. Those with AVMs in the lung face the possibility of a life threatening rupture, stroke or brain abscess-especially during pregnancy. HHT patients with brain AVMs do not generally have warning symptoms prior to a life-threatening brain hemorrhage. Heart failure is another risk HHT patients face due to high flow liver AVMs.
Regardless of location or size, abnormal blood vessels have a greater tendency to rupture and bleed compared to normal blood vessels and should be closely monitored.
Those with HHT may have blood vessel abnormalities in the:
nose, skin of the face, hands and mouth, lungs, brain, lining of the stomach and intestines (GI tract)
Prevalence
About 95% of those with HHT have recurring nosebleeds.
95% of HHT patients have telanglectases in the skin of the hands, face and mouth that generally become apparent in their 30s or 40s.
GI bleeding will develop in about 25% of HHT patients (after age 50) which can result in black stools or anemia.
30% will have one or more AVM in the lung that is life threatening should it rupture. Pregnant women with HHT are at increased risk of AVM rupture in the lung due to an increase in blood volume and cardiac output in the last trimester. Patients with lung AVMs are also at risk for stroke or a brain abscess from the lack of capillaries to filter impurities like clots, bacteria and air bubbles.
Brain AVMs are found in 15% of HHT patients and can be life threatening.
Spinal AVMs are fairly rare and cause back pain or loss of feeling/function in arms and legs.
Recurrent Nosebleeds Are Most Common HHT Symptom
Approximately 95% of HHT patients eventually have recurrent nosebleeds, with one-third having onset by the age of 10 and 90% by age 21. Other characteristics of HHT include small red to purple spots and lacy red vessels.
HHT, Women and Pregnancy
Female hormones are known to affect bleeding of abnormal HHT blood vessels. For some women, nosebleeds vary through the menstrual cycle and become worse after menopause.
Most pregnant women with HHT can expect no serious HHT-related complications. For some, new skin telangiectases are detected, while others report improvements. There is great concern for pregnant women with an AVM in their lung. During pregnancy, there is a 60 percent increase in blood circulation that is essential to the development of the baby. This increase in pressure on weak abnormal blood vessels increases the risk of a life threatening rupture in the lung. Research shows that it is safe and efficacious to perform embolization on pulmonary AVMs during the second trimester of pregnancy.
Both HHT mothers and their babies can generally expect a safe pregnancy.
Diagnosis
In the mid 1990’s scientists discovered that an abnormal gene on either chromosome 9 or 12 causes HHT. Chromosome 9 (endoglin) and chromosome 12 (activin-like kinase) tell the body to produce a substance that is involved in the formation of blood vessels. HHT is a “dominant” disorder since one abnormal copy of the gene from one parent can cause the disorder. Although there is a 50 percent chance of inheriting this abnormal gene, children who do not have it cannot pass on the disease.
In 2003, genetic testing for HHT became available at only a few genetics laboratories in the United States. The complicated family-based testing should be run, ordered and managed by an HHT Center or genetics professional. According to recently published Clinical Diagnostic Criteria, a person has HHT if they have three or more of the following criteria and are suspect if they have two or more of the criteria:
Nosebleeds are spontaneous and recurrent
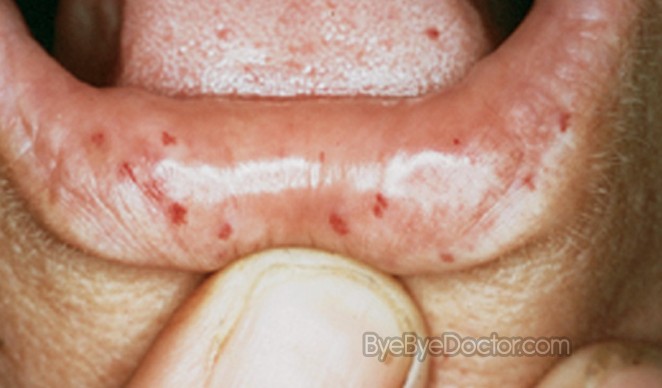
Telangiectases are prevalent at characteristic sites such as lips, oral cavity, fingers and nose
AVMs are present in lung, brain, GI, liver or spine
Family history indicates a parent, sibling or child has HHT
Interventional Radiologists Treat Malformations Nonsurgically with Embolization
The location of the telanglectases determines the course of treatment for HHT patients. Interventional radiologists treat malformations in the lung and brain using embolization.
Lung – These malformations should be treated, even prior to symptoms appearing, due to their life threatening/disabling nature. Interventional radiologists, vascular experts who treat patients internally using imaging to guide them, can permanently treat lung AVMs using a minimally invasive procedure known as embolization. During this procedure, an interventional radiologist makes a small nick in the skin, inserts a catheter into the femoral vein in the groin and then directs it to the abnormal blood vessels in the lung. Next, Dacron platinum coils are placed in the artery feeding the AVM to permanently block the blood flow to the AVM. Patients should be seen one year after treatment by the interventional radiologist to be sure the AVM has been resolved.
Patients are treated either as an outpatient (single AVM) or as an inpatient (multiple AVMs). Local anesthesia is given.
Brain – Size, structure and location in the brain impact how these AVMs are treated. Surgery, embolization and stereotactic radiosurgery are treatment options that can be used separately or in combination. Decisions about whether to treat and types of treatment should be made by a team including neurovascular neurologist, neurosurgeon, and interventional neuroradiologist.
Establishing a Treatment Plan
Currently, there are nine multi-discipline centers for management of these patients and families. It is recommended that an initial diagnosis and treatment plan should be developed for each patient by one of these centers. Centers are located at:
Mayo Clinic
Medical College of Georgia
Oregon Health Sciences University
University of California San Diego
University of Pennsylvania
University of Toronto
University of Utah
Washington University St. Louis
Yale University