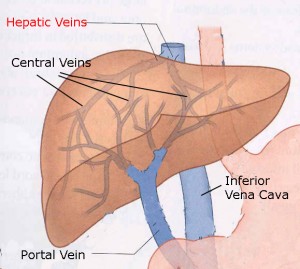
Hepatic Vein Thrombosis
Hepatic Vein Thrombosis
The causes of hepatic vein thrombosis are numerous so treatment to the disease can be quite different. Read on the following article to learn more information about the diagnosis and cure of the disease.
What is the hepatic vein?
The hepatic veins are blood vessels located in the liver. Their function is take the deoxygenated blood from the liver to the lungs. Most veins in the body contain valves to control back flow of blood. Hepatic veins do not contain valves
What is Budd Chiari syndrome?
This syndrome is a name given to a condition where the hepatic veins are obstructed by a blood clot. The syndrome classically presents with abdominal pain, fluid in the abdomen (ascites) and liver enlargement (hepatomegaly).The syndrome can present all of a sudden or gradually. It occurs in 1 out of 100,000 individuals and is more common in females. Some 10-20% also have obstruction of the other liver veins (portal vein).
What happens when the hepatic vein is blocked?
When the hepatic vein is blocked, the blood starts to pool behind it and causes a rise in the venous pressure. This causes the body to develop small channels (collaterals) to work around the blockage and take the blood back to the lungs. However, these new veins are very thinned walled and easily get engorged with blood. The constant back pressure of the blood causes veins to swell up in the entire abdomen. Some individuals develop very large hemorrhoids which can bleed severely if traumatized. These thinned wall vessels are very fragile and repeatedly rupture causing vomiting of blood, which is uncontrollable in many cases.
How does Budd Chiari syndrome present?
Budd Chiari classically presents with 3 features which include liver enlargement (hepatomegaly), distended abdomen with fluid (ascites), and abdominal pain.
Is the disorder always painful?
No. The majority of patients have a slower-onset form of Budd-Chiari syndrome. This can be painless. When the block is gradual, it allows the body to make collateral (channels) to bypass the blockage. These collaterals may be seen on a CT scan or an MRI.
What are causes of hepatic vein blockage?
The causes of hepatic vein thrombosis are numerous and include the following:
Unknown: About 30-50% of cases have no identifiable cause.
Congenital: Sometimes one may be born with a deformation of the hepatic vein and the disorder will present in childhood.
Thrombosis: Any condition which predisposes one to blood clots can cause Budd chiari syndrome. These blood clotting disorders include deficiency of Protein C and S, and anti phospholipid syndrome.
Drugs: Use of birth control pill, Pyrrolizidine alkaloids found in certain herbs (e.g., borage, comfrey) are known to cause blood clots in the hepatic vein.
Medical disorders: Conditions which increase the tendency of blood to become thick, viscous and sticky can also cause blood clots in the hepatic vein. These conditions include thrombophilia, Sickle cell anemia, paroxysmal nocturnal hemoglobinuria and Bechet’s.
Trauma: Injury to the hepatic veins can lead to blood clot formation.
Radiation injury: Prolonged exposure of the hepatic veins to radiation (when treating cancers) can also cause clotting in the hepatic veins.
Cancers: Some cancers within the vicinity of the liver can cause thrombosis or external compression of the hepatic veins. This includes cancers of the kidney, adrenal, liver, bile ducts and cancers which have spread from elsewhere in the body
Pregnancy: For some unknown reason, this condition is often seen in pregnant females.
How is diagnosis of hepatic vein thrombosis made?
Blood work: Some basic blood work will reveal abnormalities in liver function but is not diagnostic of the syndrome.
Ultrasound: This technique may reveal absence or narrowing of the hepatic vein or the presence of the large thinned wall collaterals. It may also show enlargement of the liver and the presence of fluid in the abdomen.
CT scan and MRI: These two tests can show the anatomy of the liver with remarkable resolution and reveal the presence of hepatic vein thrombosis. CT may also reveal the presence of any cancer causing obstruction of the hepatic vein.
Liver biopsy: Sometimes the cause of the liver failure may not be obvious and a liver biopsy is indicated
How does one treat hepatic vein thrombosis?
Treatment of hepatic vein thrombosis is difficult and involves the following:
Medications: For those who have fluid accumulation in their abdomen, water pills may help. However, this is only transient therapy and does not always work.
Blood thinners: Unlike elsewhere in the body, blood clots in the hepatic vein do not generally resolve and so the role of blood thinners is still undecided. Clot blusters have been tried but the results have been disappointing. Since these patients have a tendency to bleed, use of blood thinners and clot busters should be used with extreme caution.
Surgery: Sometime surgery can be done to bypass the blockage in the hepatic vein. However, the surgery is very complex and when done in the presence of liver dysfunction, the results are poor.
TIPS: This non surgical procedure is done by a radiologist who places a stent (metallic tube) in the hepatic vein. However, TIPS created shunts do have a habit of re blocking.
Liver transplantation is an effective treatment for Budd-Chiari. However, liver donors are rare and there is long waiting list. In addition, liver transplantation is no walk in the park. It is complex surgery and requires taking toxic drugs for the remainder of one’s life. Even after transplantation, the liver may be rejected and there are other complications including bleeding and arterial thrombosis. Up to 10% of patients may have a recurrence of Budd-Chiari.
What is prognosis of patients with hepatic vein thrombosis?
If the individual has minimal symptoms and the liver is functioning well, the majority of patients survive for at least 10 years after the diagnosis. However, if symptoms are present and the liver is destroyed, the prognosis is very poor. If the hepatic vein is blocked by a cancer, then most individuals are dead within 1-3 years.
For those with no symptoms, life will go on as normal.